Q & A session with cardiovascular physiologists DeWayne Townsend (DVM, Ph.D.) and Adam Goodwill (Ph.D.), plus ADInstruments support specialists on frequently asked questions about cardiac pressure-volume (PV) loop studies.
Please note, the following questions were asked during our webinar on Cardiac PV Loop Data Analysis: Tips and Tricks. See here to watch the webinar on-demand.
Q & A session overview:
- Anesthetics
- Positioning the catheter in the ventricle
- Apical vs. carotid approach
- Catheter function and calibration
- Fluid management
- Animal ventilation
- Inferior vena cava occlusions (IVCO) and abdominal compressions
- Experimental validity
- PV loop parameters (load-dependent and load-independent)
- Right ventricular PV loop measurements
- Measuring PV loops in ex-vivo heart preparations
- Alternative techniques to PV catheters
- Additional resources
Anesthetics
Is there a preferred anesthetic to use for PV loop measurements? As several anesthetics can depress CV function.
Adam: Historically, our group has used a combination of alpha-chloralose and morphine as this provides a stable plane of anesthesia without significantly depressing CV function. However, for many, inhaled anesthetics are preferable. While you will never be able to fully avoid the CV impact of isoflurane, dosing the animals with a potent analgesic such as buprenorphine prior to the procedure allows you to maintain an appropriate plane of anesthesia at a lower total inhaled gas volume. This minimizes the impact that the anesthetic will have on the preparation.
What is your preferred anesthesia for maintaining stable respiration during an experiment?
Adam: We have always had success with isoflurane.
What are your thoughts on heart rate as a function of anesthesia effect?
DeWayne: Much of the reductions in heart rate induced by anesthesia is secondary to depression of the sympathetic nervous system. Thus, heart rate can be a reasonable measure of cardio-depression. For the mouse resting heart rates >500 bpm are generally expected. However, it is important to note that various genetic models might have alterations in heart rate independent of the anesthesia used.
Do you recommend maintaining a constant temp and anesthesia during the experiment?
DeWayne: Yes! This is absolutely necessary. Changes in body temperature are critical factors defining cardiac functionality. I recommend including body temperature on a monitoring sheet to 1) have a record of this parameter and 2) to remind the user to keep the body temperature around 37°C.
What is the ideal dose of isoflurane for mice and rats for PV loop experiments?
Adam: I don’t honestly believe that there can be a correct answer to this question. There are simply too many factors that go into consideration including species, strain and disease state. Anesthesia should be maintained at the lowest possible dose while still providing an adequate plane for the procedure to be fully humane. This is best accomplished by continuous monitoring.

Pro Tips:
- Proper anesthesia is an essential part of obtaining high-quality PV-loops. There are many different combinations present in the literature all of which have some degree of cardio-depressive actions. I personally prefer to use inhalant anesthesia for the simple reason that you can titrate it to the depth you need.
- During periods of surgical manipulation, it is necessary to maintain a surgical plane of anesthesia; however, this degree of anesthesia will depress cardiac function. Once surgical manipulations are completed, a surgical plane of anesthesia is no longer needed and the level of anesthetic can be lowered to achieve a plane of deep sedation that has less cardio-depressive actions. Of course, this must be done very carefully to ensure that sufficient anesthesia is present.
- Every anesthetic system is a little different so the doses of anesthetic must be guided by careful monitoring of the experimental subject. For example, with my system, 2% isoflurane is sufficient for surgical procedures and 1% provides enough anesthesia to maintain sedation throughout the protocol. The reduction in anesthesia is done once surgical manipulations are complete and is associated with a significant improvement in contractile function.
Positioning the catheter in the ventricle
Any recommendations to make sure the catheter remains in the same position throughout the experiment? Particularly for swine with a catheter placed percutaneously via the carotid artery.
DeWayne: In the carotid artery studies I’ve done, we used an introducer that provided enough resistance that the catheter stayed in place.
Adam: Our group typically approaches via a transmural insertion through the ventricle. However, regardless of the avenue, our catheters are introduced through an introducer sheath with an included hemostatic control valve.
Do you remove the epicardium to insert, this could have a major effect on function?
DeWayne: I do not remove the epicardium as doing so would damage the heart. I do however remove the pericardium during the apical approach. This may have some impact on certain aspects of cardiac function, but it is done equally to all experimental groups so any effect will not present a systemic bias. Removing the pericardium simplifies the apical catheter placement by preventing the pericardial membrane from covering the site of the stab incision. Furthermore, the pericardium is easily damaged when entering the mouse chest and complete removal increases reproducibility.
Many times I have experienced end-diastolic signal interference in my loops, due to the proximity of the catheter to the mitral valve (apical approach).
Do you have any tips for improving my catheter positioning towards the aortic valve?
DeWayne: The best advice I can give is point the catheter toward the aortic valve. It may be helpful to do a careful dissection to become familiar with cardiac anatomy. It is critically important that the catheter insertion site be slightly lateral to the apex of the heart. You want your catheter to move parallel to the interventricular septal wall. If you maintain this along the axis of the heart, your catheter will (most likely) avoid the chordae tendineae associated with the mitral valve.
We put a catheter through the apex to measure LV loops, however, the resulting loop shape shows very narrow or small in the mouse model. What is the reason for this?
DeWayne: Narrow loops suggest that something is amiss with your volume signal. The volume is a calculated parameter that has several inputs depending on the system you are using. An error in setting any number of these parameters can result in a low volume signal. It is also possible that the catheter itself is damaged, the electrode connections sensing or generating the electrical field are usually the first indication of a damaged catheter.
Related: Step-by-step surgical instruction videos for invasive pressure and pressure-volume studies »
Apical vs. carotid approach
How can I keep the catheter in place when using the apical approach? Is tissue glue recommended?
ADI Team: Millar advises against using any sort of adhesive with the catheter. A piece of tape or malleable clay that you keep off the heating pad are common ways to secure a catheter in place.
DeWayne: I find that suture spools or other relatively lightweight objects can keep the catheter in place. The most important part of this is that the “memory” of the catheter needs to be pretty close to its final position in the animal, you can not rely on the rodent ventricle to hold a PV catheter that wants to be pointing another direction.
Adam: Once the catheter is positioned and affixed (typically through a purse-string suture), we tape the exposed catheter to the animal or some region of the table.
By using the carotid approach, I usually observe negative EDP values, even when trying different positions. However, the same does not happen when the apical approach is performed. Any tips?
ADI Team: Were there any variations in how you prepped the catheter for these two surgeries? Normally, when we see negative pressure values, the cause is related to how the catheter was pre-soaked and zeroed. Millar and ADInstruments recommend pre-soaking the catheter for at least 30 minutes in body temperature isotonic saline, and moving the sensor to be just under the surface of the saline before zeroing the catheter.
DeWayne: It is possible that if the animal is exerting a significant amount of respiratory effort that you might be measuring changes in intrathoracic pressure. This, of course, should display a periodicity that matches respiration.
The discussion of the surgical approach suggested aorta insertion. But it is easier to go in through the carotids, my question is which is better right or left carotid for insertion.
DeWayne: The right carotid artery gives you a straighter line into the left ventricle and is generally preferred. However, it is possible to place the catheter from the left carotid artery.
What is your opinion of how much normal physiologic parameters change when using the open chest method? We have always thought the retrograde approach was superior because of this issue.
Adam: With the caveat that this is entirely based on opinion, you will either examine effects in an anesthetized animal with an open chest or an anesthetized animal with a catheter coming through a valve. In either scenario, the data should be treated as being reflective of their own specific conditions. I can’t make an argument to say that one approach is closer to what is found in a conscious ambulatory state than another.
Read more: Left ventricular catheterization - Apical vs. carotid approach
Catheter function and calibration
Are there differences in pressure sensor types offered by vendors that could help mitigate ventricular pressure artifacts from cardiac structures?
ADI Team: Most solid-state pressure sensor catheters on the market use the same sensor orientation as Milar. Fine adjustments in catheter position, such as rotating, advancing, or withdrawing the catheter slightly, is what most users in our experience use to prevent ‘sensor strike’ artifacts in their Pressure and PV data.
You mentioned that catheter size impacted SV and Diastolic volume by occluding outflow. Is potential leakage through the Aortic valve also a concern? Do you have representative PV loops showing this effect?
DeWayne: We cannot rule out aortic valve leakage. However, this difference was most striking in a transgenic model that had notably small hearts. It was less evident in mice with larger hearts. These observations led to the notion that it was an outflow tract obstruction; although it is possible that some combination of small aortic valve and catheter may lead to valvular insufficiency. Unfortunately, I don’t have the PV loops showing this effect.
How is ventricular volume measured?
ADI Team: Millar Catheters use the Conductance method to measure the ventricular volume. This scientific paper HERE (Pacher et al. 2008) covers the basics of the conductance volume method.
What’s the best method for calibrating your volume signal using a conductance catheter?
ADI Team: The analysis that is desired should be considered when developing your protocol. If ESPVR and EDPVR are the only parameters of interest, you really do not need to do any saline bolus or cuvette calibrations as these are purely a relationship change measure occurring during a procedure (occlusion). EF%, CO estimates, and SV are common parameters that require volume measurements, in which the most accurate volume data will be produced by doing the saline and cuvette calibration for each animal, and is recommended by Millar and ADInstruments. Depending on the protocol and treatments, researchers will sometimes choose to use cuvette calibration values from a few animals of a population and apply them across the population to speed up their procedures, but care should be taken if you choose to use a representative value when individual physiological differences are common. The ADInstruments Webinar located HERE covers this topic in further detail.
Do you have any recommendations for filtering (smoothing) methods, especially for volume traces?
ADI Team: Normally, filtering should not be required provided potential sources of noise are kept physically distant from the catheter’s adapter cable and the subject. However, the volume signal can be susceptible to 60 Hz noise, so if you experience this type of noise applying a 50 Hz LowPass filter will help. You may also consider using a Smoothing Filter with 19 or 21 samples for 1000 s/s sampling rate to improve your loops without changing their shape.
What are the characteristics of conductance and admittance techniques, which are available for PV loops acquisition?
ADI Team: Both systems (Admittance and Conductance) utilize a high-frequency low-amplitude constant current to develop an electromagnetic field for sensing LV volume. Catheters using either method can be used to acquire PV loop, and the primary difference that a user will notice is the unique way each method removes the parallel conductance (Vp) contributed by the myocardia from the measured LV volume. With Conductance systems, a small saline bolus is introduced into the Jugular Vein for every subject to temporarily vary the conductance of the LV blood pool. This variation is used to calculate and remove the effectively constant Vp value present with this method in the ADInstruments PV-Loop module. Meanwhile, admittance systems take advantage of the fact that blood is purely resistive at the frequencies used in the magnetic field, while the myocardium has both resistive and capacitive properties. This difference in the properties of the blood and heart, along with some knowledge about the myocardial capacitance, are used to separate the measured blood and heart conductance.
Is it advisable to calibrate the PV loop data with LV volumes obtained by Echocardiography for the same animal?
ADI Team: If you choose to use this option in the PV-Loop module, yes, you will need to use Echo data from the same animal to calibrate. Variation can be quite dramatic between animals from the same population, especially in a diseased model, which would in turn negatively impact the accuracy of the resulting data.
Is there a specific amount of saline you should inject for saline calibration?
ADI Team: Millar recommends the following:
- Mice: 15-30%; 5-10 µL
- Rats: 15-30%; 20-40 µL
- Large Animals: 15-30%; 0.25 mL per Kg of body weight
Additionally, the pressure signal should stay steady, and the volume signal should have a roughly linear increase in the max volume point over a period of 10-15 loops. Each laboratory likely needs to refine this for their protocols, but consistency in injection speed, volume, and salinity are key.
What are signs on the recording that there is a problem with the catheter itself?
ADI Team: When it comes to the pressure signal, the signs you will see in the suggesting that the catheter has failed are as follows:
- Catheter continues to have large baseline oscillations (>6 mmHg) after pre-soaking the catheter in body temperature, isotonic saline for 30 - 45 minutes or experiences large baseline drift, again >6 mmHg, when it is placed in the subject.
- Catheter pressure signal suddenly shifts up or down by more than >10 mmHg after the catheter has been properly positioned in the LV.
- Pressure signal constantly reads out of range.
When it comes to the volume signal a failed catheter will simply read out of range on all or some of the volume segments.
In your experience, how real are negative minimum pressures? Is there a threshold below which we need to consider if something is wrong with the catheter?
ADI Team: In our experience, negative pressure values <4 mmHg are due to either small variations in the zeroing and calibration process and are not something to be concerned about. If the negative pressure values are over that amount, an error has been made during the zeroing process, and said process will need to be reaccomplished.
Fluid management
Do you provide the fluid intraperitoneally (I.P.)?
DeWayne: IV fluid is preferred as it will directly contribute to the intravascular volume. The use of a colloid (such as 10% albumin) IP could pull volume out of the intravascular space, which would not be ideal.
Would you recommend IV continuous infusion of albumin during the experiment instead of IV bolus?
DeWayne: I deliver a bolus over 10 minutes.
Which vein are you using for albumin bolus?
DeWayne: The right external jugular vein is pretty prominent in the mouse.
Do you have any suggestions on IV fluid replacement for pigs?
Adam: In a carefully performed procedure, significant fluid loss from a pig should be relatively minimal. In our procedures, to minimize fluid loss, all surgical sites are approximated and/or covered with plastic wrap through the procedure to minimize evaporative loss. If there is a concern about significant fluid loss, IV infusion of volume expanders like Hespan can be employed. However, you should exercise caution in their use as you may bias the dataset by taking the animal to a supraphysiologic volume.
Could you consider resuspended donor erythrocytes to maintain blood volume?
Adam: Possibly although this would have to be done extremely carefully to avoid hemolysis.
When you inject hypertonic saline, it can change heart load. How do you avoid that?
ADI Team: In our experience, the impact on preload can be minimized by using the smallest amount of saline possible to achieve the desired increase in max pressure values and shift of the PV loops. The recommended volume and concentration ranges for the various animal models are as follows:
- Mice: 15-30%; 5-10 µL
- Rats: 15-30%; 20-40 µL
- Large Animals: 15-30%; 0.25 mL per Kg of body weight
Additionally, delivering the bolus quickly over the timeframe of 10-15 beats can minimize its effect on preload.
Animal ventilation
I'm wondering if it's necessary to intubate in an open chest setting? I was taught that intubation was not required as a quick analysis for 10min...but it doesn't seem to be recommended even in this event
DeWayne: Open chest animals should always be intubated. If you open the chest without ventilation, gas exchange will cease. Over the course of a few dozen seconds, the animals will become hypoxic with severe acidosis. I would be surprised if it survived for a few minutes and any data collected would be highly variable as the animals are rapidly decompensating.
Can you apply the ventilator to acquire load-independent measures (without IVC)?
DeWayne: While the ventilator does create small changes in left ventricular loading, in my experience they are not of sufficient magnitude to be useful in calculating load-independent measures of contractility.
We have found that some mice continue to breathe even when we turn the ventilator off - thoughts?
DeWayne: This generally means that they are hypoventilated. Increasing either the rate or peak pressure/volume should remove the respiratory drive. Which should give you 3-4 seconds of apnea when you stop the ventilator.
How could I generate an apnea when the chest is not open?
DeWayne: If you are not ventilating, it is not possible to accurately generate an apnea.
Gasping always occurs during our experiment. How do I stop this from happening?
DeWayne: Gasping is a sign of respiratory distress. Increase the ventilation to the animal by increasing breathing rate, peak pressures/volumes, or adding positive end-expiratory pressure will all help to increase ventilation.
Inferior vena cava occlusions (IVCO) and abdominal compressions
For cava occlusion in closed-chest pigs, would a balloon cava occlusion work?
Adam: Yes. We advance a fogarty catheter into the IVC and inflate the balloon.
How many seconds is required for an IVC occlusion to get a smooth loop shift?
Adam: This somewhat depends on heart rate but a smooth IVC occlusion should be visible on the very next beat.
How much should pressures decline in a large animal when doing a caval occlusion?
Adam: This will depend on how long you perform the occlusion. Systolic pressure will drop continuously through an occlusion and can easily reach a point that is not compatible with life. We generally don’t allow an occlusion to go beyond 10 or so cardiac cycles for this reason. Over the course of that occlusion. Although there isn’t an exact number, the pressure should visibly drop with each cardiac cycle.
During the experiment, how does one deal with changes in muscle contribution during an occlusion? Does that have an impact on how you interpret the outcome?
ADI Team: The Conductance method of volume measurement assumes a constant contribution (called parallel conductance or Vp) by the myocardia. This assumption is supported by the findings of the paper located HERE (Georgakopoulos et al. 2000).
Have you observed a biphasic pattern when performing an IVC occlusion? If so, which slope do you use?
Adam: A biphasic pattern may relate to the system responding to decreased systemic pressure (baroreceptor responses). To avoid these, perform as brief an occlusion as you reasonably can. Regarding analyzing data, the early response would be the response that occurred independent of baroreceptor signaling but appropriately identifying the point of delineation in the data would be an extreme challenge.
Should all measures of contractility (Ees, PRSW, dp/dtmax-EDV) be analyzed from one IVC analysis or we can play around and remove loops to get a good R squared for each measure separately? And what is the acceptable R squared for IVC analysis?
Adam: I wouldn’t advocate for removing data without justification. In our experience, during IVC occlusion, you do sometimes get loops that are clearly the result of a signal issue (a loop that crosses itself or one where the shape radically shifts). In those instances we will exclude a loop. For our data analyses, we commonly limit ourselves to the first loop that is not reflective of occlusion and a small number of occlusion loops thereafter. Our cutoff for R squared is usually 0.95 or above.
Experimental validity
In your experience, what is a good N number of mice to evaluate?
Adam: This is dependent on your outcome variable of interest and the anticipated variation in your dataset. Ultimately, you will need to perform power analyses to get an answer of value.
PV loop parameters
Why is ESV identified as the point of the end of isovolumic relaxation (A), and not as a point of the aortic valve closure (F)? Even though the isovolumic relaxation suggests that the volume does not change, the in vivo data shows that the volume usually changes in a range of 10-15% during this period.
Adam: The end-systolic pressure-volume point is point F (view the webinar for more information).
On the PV loop, where exactly is the EDPV point?
Adam: Point C on the example loop in (view the webinar for more information).
On the Starling curve, why is stroke volume less influenced by heart rate than cardiac output?
Adam: This comes back to the calculation of cardiac output (SV x HR).
Q. Does heart rate affect ESPVR?
Adam: Heart rate dependent changes in inotropy are termed Bowditch or Treppe effects. They have been documented experimentally but their physiologic relevance is equivocal.
Right ventricular PV loop measurements
What technique do you use if you want to study the right ventricle? Can you use the closed chest method?
ADI Team: Yes, by going through the Jugular Vein. Introduction of the catheter is more difficult due to the structure of the venous system, but has been reliably published on. However, most researchers studying the RV will use the open chest surgical approach.
I found that it is more difficult to get appropriate volume (CO and EF) and sometimes the HR when experimenting in RV compared to LV, any suggestions on how to improve these parameters in the RV?
ADI Team: The ADInstruments PV Loop module versions 2.5 and later have an improved End Systole detection algorithm that was primarily designed for use with RV data, but also works well for non-typical RV data. To learn more about this new algorithm, review the video located HERE.
Measuring PV loops in ex-vivo heart preparations
Can you measure PV loops in ex-vivo preparations reliably?
ADI Team: Yes, in a working heart preparations with systems such as those offered by Radnoti. The Jove Article and Video located HERE demonstrates how this can be done.
Any tips for measuring PV loops in Langendorff perfused hearts? How does this compare to in situ?
ADI Team: This cannot be done in a Langendorff prep, and can only be done in a working heart preparation (antegrade rather than retrograde perfusion).
Alternative techniques to PV catheters
Between the Echo and PV loop techniques, which is more informative and technically easy?
ADI Team: This question was addressed by Dr. Goodwill during the webinar, between the 1:30 and 3:30 time points. A recording of the webinar can be found HERE for your review.
Additional resources:
- Step-by-step surgical instruction videos for invasive pressure and pressure-volume studies »
- Cardiac PV Loop Data Analysis: Tips & Tricks (Webinar) »
- PV Tips and Tricks: Expert advice for measuring pressure-volume loops in mice »
- Optimizing your Blood Pressure and Pressure-Volume Recordings »
- Cardiovascular Assessment of Pressure-Volume and Blood Pressure »
- Introduction to PV loops: Understanding the PV loop and measures of cardiac function »
- Troubleshooting your Millar Catheter: Three common problems and how to fix them »
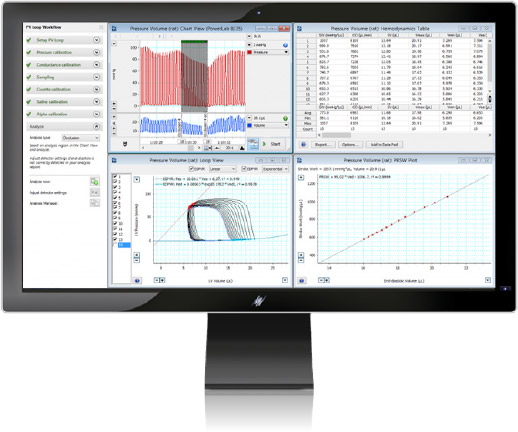
LabChart software – PV Loop Module for left and right ventricle studies
The PV Loop Analysis Software Module for LabChart is specifically designed for the analysis of in vivo ventricular pressure-volume data in small and large animals, or ex vivo, using working heart systems.
Our PV loop module provides workflows for acquiring PV loop data from small and large animal models as well as tools for analyzing left and right ventricular PV data in real-time or post-acquisition. Contact us for more information.